Introduction to Global Health
EVEN 2909: Introduction to Sustainability Engineering
University of Colorado Boulder
Course Overview
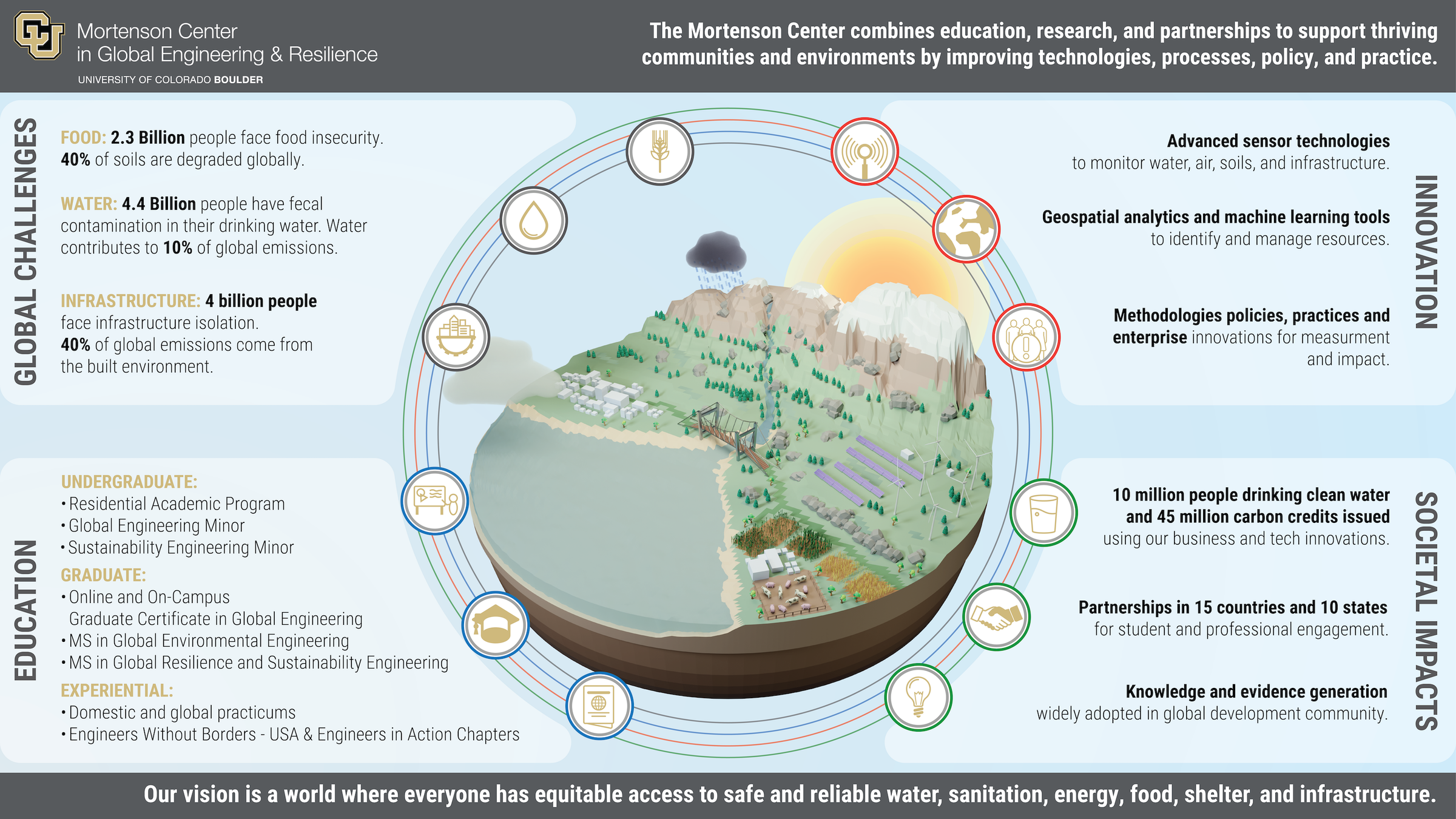
Lecture Overview
This lecture introduces the professional field of Global Health, with a particular focus on how it connects to sustainability engineering. We will examine community environmental health -- the area where engineers most frequently contribute -- and explore how disease, poverty, water, sanitation, and air quality intersect with the engineering challenges you will encounter throughout this course.
We will examine published peer-reviewed studies of global health interventions. Learning how to search for, read, and analyze these kinds of studies is fundamental to being conversant in global health and sustainability engineering.
Key topics include the determinants of health, the global burden of disease, communicable disease transmission, and the environmental health factors -- air quality, water, and sanitation -- that sustainability engineers are uniquely positioned to address.
Evan Thomas
Professor
- Environmental Engineering Program
- Civil, Environmental and Architectural Engineering Dept.
- Aerospace Engineering Sciences Department
Mortenson Endowed Chair in Global Engineering
Director, Mortenson Center in Global Engineering
University of Colorado Boulder
- PhD, Aerospace Engineering Sciences, 2009
- MS, Aerospace Engineering Sciences, 2006
- BS, Aerospace Engineering Sciences, 2005
- BS, Broadcast Journalism, 2005
Oregon Health and Science University
- MPH, Master in Public Health, 2014
Fletcher School at Tufts University
- Global MBA, 2022
NASA Johnson Space Center, Aerospace Engineer, 2004-2010
Portland State University, Assistant/Associate Professor, 2010-2018
Virridy Inc, Founder and CEO, 2012 – Present
Manna Energy Limited / DelAgua Health, Founder, COO, 2007-2016
~80 journal articles, 10 patents, professional work in 16 countries




The Current State of Global Health
2025–2026: A period of unprecedented disruption to global health infrastructure.
USAID Shutdown
Timeline
- Jan 20, 2025: Executive Order freezing all foreign assistance funds for 90 days, including PEPFAR
- March 2025: Termination of 83% of USAID's 6,300 global initiatives
- Staff cut from 10,000 to 15 personnel
- Feb 2026: Congress passed $50B foreign aid bill to begin reinvestment
Projected Impact
- 9.4 million additional deaths projected by 2030 (The Lancet)
- 500,000–1,000,000 lives lost in 2025 alone (Center for Global Development)
- 2.3 million people on antiretroviral treatment lost support
- 12.5–17.9 million additional malaria cases projected
- 2.4 million people in Yemen lost food assistance
US Withdrawal from the WHO
What Happened
- Jan 20, 2025: Executive order giving one-year notice of withdrawal
- Jan 22, 2026: US formally withdrew from the WHO
- US historically contributed ~15% of WHO's total budget (~$1.28 billion annually)
- WHO cutting ~2,371 staff (25% reduction) by mid-2026
Consequences for Global Health
- Global Influenza Surveillance and Response System (GISRS) disrupted — seasonal flu vaccine formulation at risk
- 50-country disease surveillance network dismantled
- Emergency outbreak response time reverted from <48 hours to >2 weeks
- Pandemic preparedness infrastructure weakened
EPA Rollbacks, CDC Cuts & Domestic Health
EPA Regulatory Rollbacks
- 31 climate, air, and water pollution regulations rolled back
- Emissions reporting requirements for CO2, methane, and other GHGs eliminated
- Coal-fired power plant emission restrictions dismantled
- Air pollution-related deaths projected to increase by tens of thousands per year
CDC Budget & Workforce Cuts
- Proposed 53% budget reduction for FY 2026
- ~25% of CDC workforce cut by end of 2025
- 42,000 jobs lost nationwide if proposed cuts adopted
- 60+ CDC programs eliminated, including global HIV/AIDS prevention and global immunization
- Morbidity and Mortality Weekly Report (MMWR) staff fired
Surveillance & Preparedness
- 12+ health tracking programs eliminated (deaths, disease trends)
- Disease detectives, outbreak forecasters, and data offices cut
- Public Health Emergency Preparedness funding cut 52%
- Weakened capacity for early detection, outbreak investigation, and pandemic preparedness
Implications for Sustainability Engineers
Funding Landscape Shift
Traditional USAID-funded pathways for global engineering projects are disrupted. New funding models needed — carbon credits, private sector, multilateral alternatives.
Surveillance Gaps
Engineers working in water, sanitation, and environmental monitoring face a world with weaker disease surveillance and slower outbreak response.
Domestic & Global Nexus
EPA rollbacks demonstrate that environmental health is not just a developing-country issue. Air and water quality challenges affect communities everywhere.
Local Capacity Building
With reduced external support, building local technical and institutional capacity is more critical than ever for sustainable health outcomes.
Data & Evidence
Loss of federal data collection increases the importance of independent monitoring, sensor networks, and digital MRV systems.
Discussion
How should the sustainability engineering community respond to these changes? What role can universities and the private sector play?
Intro to Global Health
Part 1 — Overview
What is Global Health?
"An area for study, research, and practice that places a priority on improving health and achieving equity in health for all people worldwide. Global health emphasizes transnational health issues, determinants, and solutions; involves many disciplines within and beyond the health sciences and promotes interdisciplinary collaboration; and is a synthesis of population-based prevention with individual-level clinical care." — Consortium of Universities for Global Health
Overview Objectives
Define the determinants, including social and economic, that impact health.
Highlight the differences in disease and life expectancy between high- and low-income countries.
Identify some of the dynamics in developing countries that impact health trends.
Key Concepts
The determinants of health
The measurement of health status
The importance of culture to health
The global burden of disease
Key risk factors for health problems
Organisation of health systems
Disciplines: Public Health, Public Policy, Medicine, Social Sciences, Behavioural Sciences, Law, Economics, History, Engineering, Biomedical Sciences, Environmental Sciences, Anthropology
Disease & Determinants of Health
Diseases Disproportionately Impacting Developing Countries
- Malaria
- Diarrhea
- Pneumonia
- HIV / AIDS
99% of the children under the age of 5 who die every year lived in developing countries.
Determinants of Health
- Genetics
- Age
- Gender
- Lifestyle choices
- Community influences
- Income status
- Geographical location
- Urbanization
- Climate Change
- Governance
- Culture
- Environmental factors
- Work conditions
- Education
- Access to health services
Multi-sectoral Dimension of the Determinants of Health
Malnutrition
More susceptible to disease and less likely to recover
Cooking with wood and coal
Lung diseases
Poor sanitation
More intestinal infections
Poor life circumstances
Commercial sex work and STIs, HIV/AIDS
Advertising tobacco and alcohol
Addiction and related diseases
Rapid growth in vehicular traffic
Road traffic accidents
Governance & Armed Conflict
Governance
Governance has a direct impact on socioeconomic status, health inequalities, and development
- Allocation of Resources
- Control of policy
- Trade agreements
- Regional politics
- Abuse of power
- Education
Armed Conflict
The Results:
- Disparities over resources and power
- Broken relationship with neighboring countries
- Lack of development
- Inequality along race/gender lines
- Resources diverted from health care to support conflict
- Displacement
Health Implications:
- Malnutrition
- Diarrhea
- Respiratory infections
- AIDS
- Extreme poverty
- Negative long-term effects on health
Intro to Global Health
Part 2 — Global Burden of Disease
Explore the Data
Interactive tools for exploring the Global Burden of Disease: GBD Compare | SDG Visualizations | Our World in Data
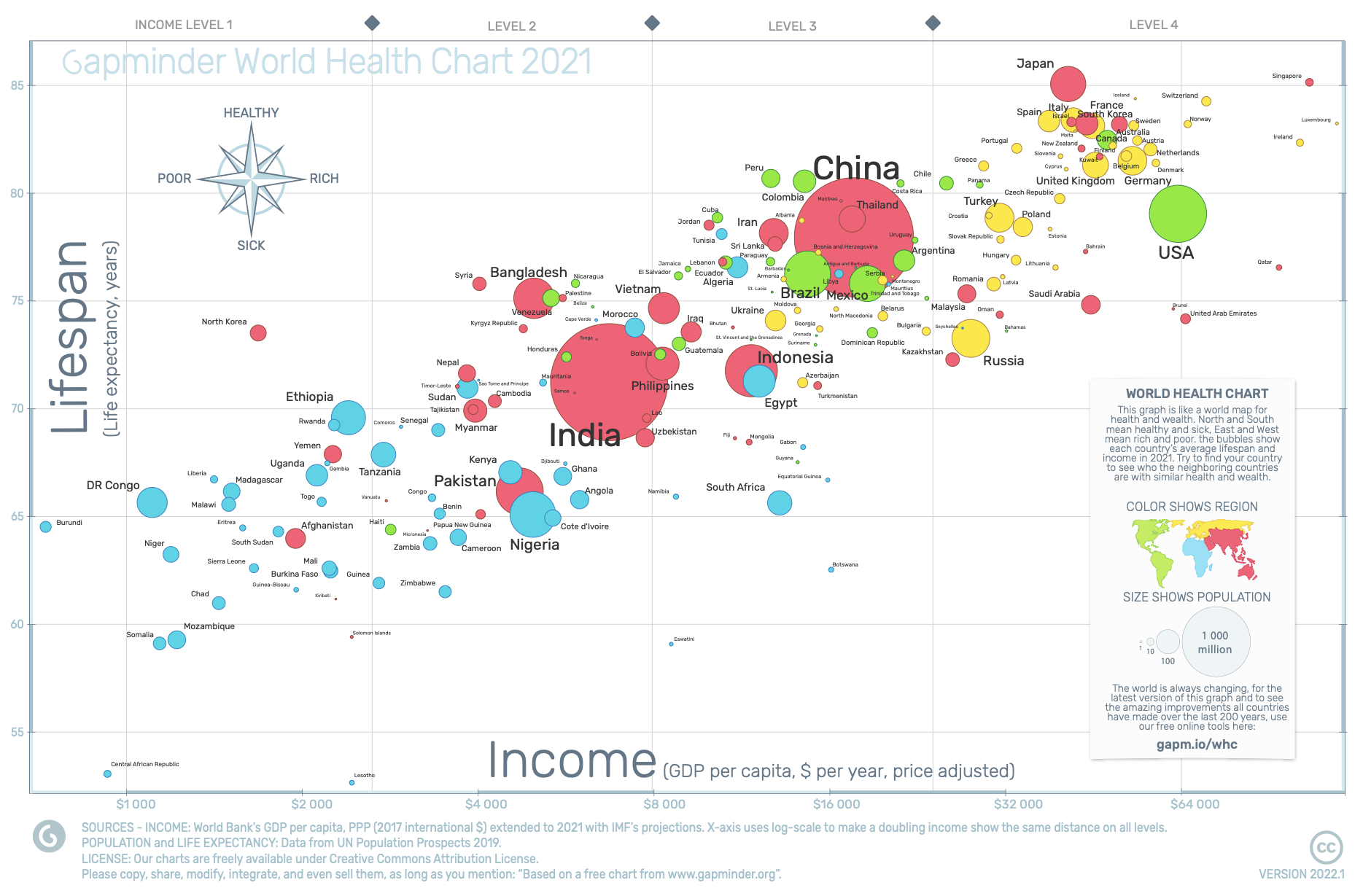
Health & Income of Nations
Life expectancy vs. GDP per capita. Bubble size = population, color = region. Source: World Bank / UN, 2023.
Global Mortality Among Children Under 5
Total deaths by cause, 1990–2021. Sources: IHME GBD 2021, UNICEF IGME 2024, WHO Global Health Estimates.
Child Mortality in Sub-Saharan Africa
Total under-5 deaths by cause, 1990–2021. Sources: IHME GBD 2021, WHO Africa Region, UNICEF IGME 2024.
Extreme Poverty by Region
People living below $2.15/day (2017 PPP). Sub-Saharan Africa is the only region where absolute numbers are rising. Source: World Bank, 2024. By 2030, 9 in 10 people in extreme poverty will live in Sub-Saharan Africa.
Per Capita CO2 Emissions
High-income countries have the highest per capita emissions, while low-income countries with the greatest disease burden contribute the least.
Global Burden of Disease
DALYs per 100,000 from all causes. Sub-Saharan Africa and South Asia bear the highest disease burden.
Undernourishment
Share of population with insufficient caloric intake. Malnutrition is a key determinant of susceptibility to disease.
Child Mortality
4.9 million children under age five died in 2022, 13,000 every day.
99% of children who die under the age of 5 are in low and middle income countries.
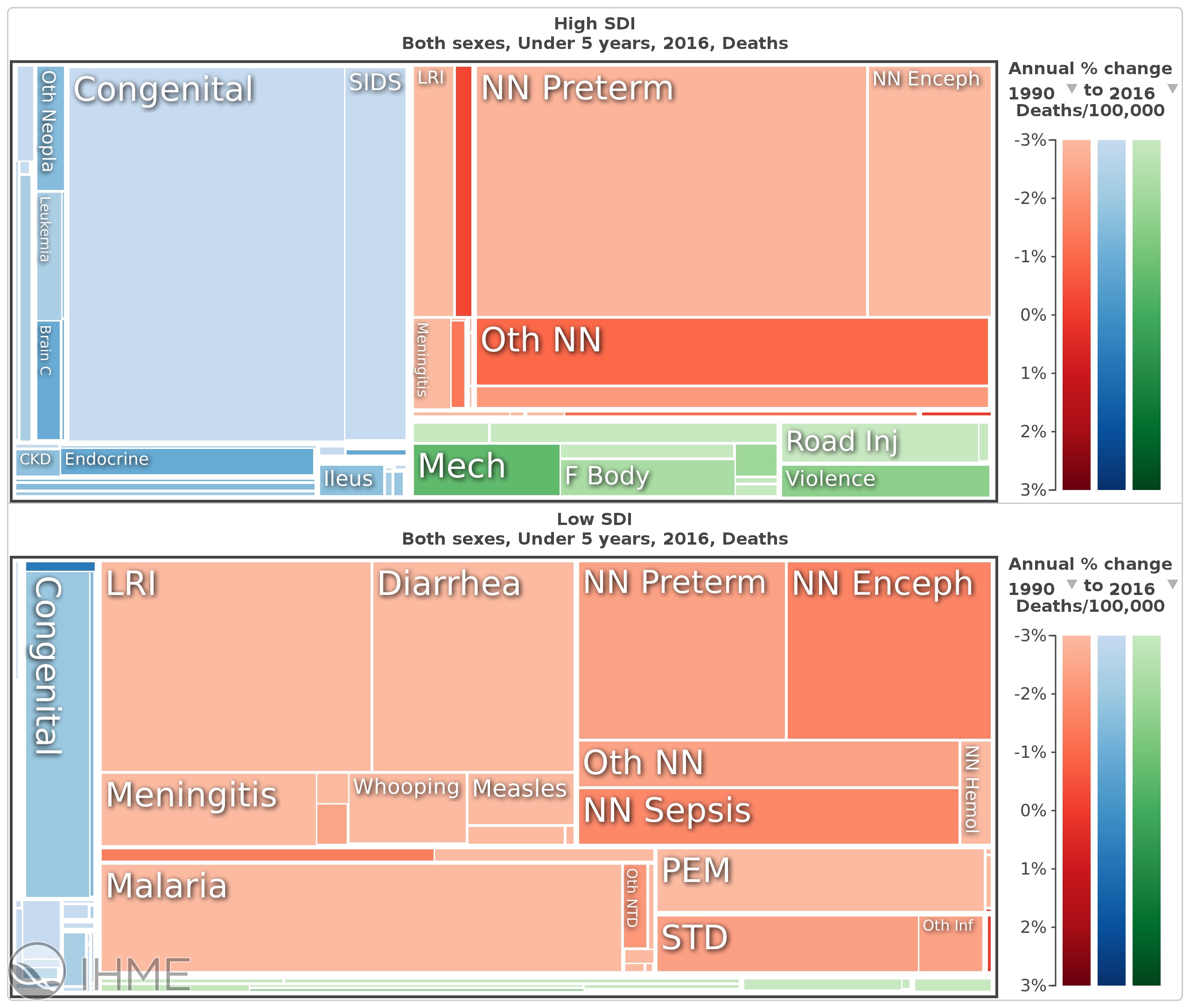
Communicable Diseases
Communicable Diseases
Defined as:
"Any condition which is transmitted directly or indirectly to a person from an infected person or animal through the agency of an intermediate animal, host, or vector, or through the inanimate environment."
Transmission is facilitated by the following (IOM):
- More frequent human contact due to:
- Increase in the volume and means of transportation (affordable international air travel)
- Globalization (increased trade and contact)
- Microbial adaptation and change
- Breakdown of public health capacity at various levels
- Change in human demographics and behavior
- Economic development and land use patterns
Modes of Transmission
Direct Transmission
- Blood-borne or sexual – HIV, Hepatitis B, C
- Inhalation – Tuberculosis, influenza, anthrax
- Food-borne – E. coli, Salmonella
- Contaminated water – Cholera, rotavirus, Hepatitis A
Indirect Transmission
- Vector-borne – malaria, onchocerciasis, trypanosomiasis
- Fomites
Zoonotic Diseases
Animal handling and feeding practices (Mad cow disease, Avian Influenza)
Impact of Communicable Diseases
Disease Burden
CDs account for about 30% of the global burden of disease and 60% of the burden of disease in Africa.
CDs typically affect low-income and middle-income countries disproportionately.
- Account for 40% of the disease burden in low and middle income countries
Most communicable diseases are preventable or treatable.
Social Impact
Disruption of family and social networks
- Child-headed households, social exclusion
Widespread stigma and discrimination
- TB, HIV/AIDS, Leprosy
- Discrimination in employment, schools, migration policies
Orphans and vulnerable children
- Loss of primary caregivers
- Susceptibility to exploitation and trafficking
Interventions such as quarantine measures may aggravate the social disruption
Economic Impact
At the macro level:
- Reduction in revenue for the country (e.g. tourism)
- Drop in international travel to affected countries by 50-70%
- Malaria causes an average loss of 1.3% annual GDP in countries with intense transmission
At the household level:
- Poorer households are disproportionately affected
- Substantial loss in productivity and income for the infirmed and caregiver
- Catastrophic costs of treating illness
Malaria
In 2022, there were an estimated 249 million malaria cases worldwide
- Causes 30% of low birth weight in newborns globally
In 2022, malaria killed an estimated 608,000 people. Malaria kills a child under 5 approximately every minute
40% of the world's population is at risk of malaria. Most cases and deaths occur in Sub-Saharan Africa.
Malaria is the 9th leading cause of death in LICs and MICs
- 11% of childhood deaths worldwide attributable to malaria
- SSA children account for 82% of malaria deaths worldwide
Source: WHO World Malaria Report 2023
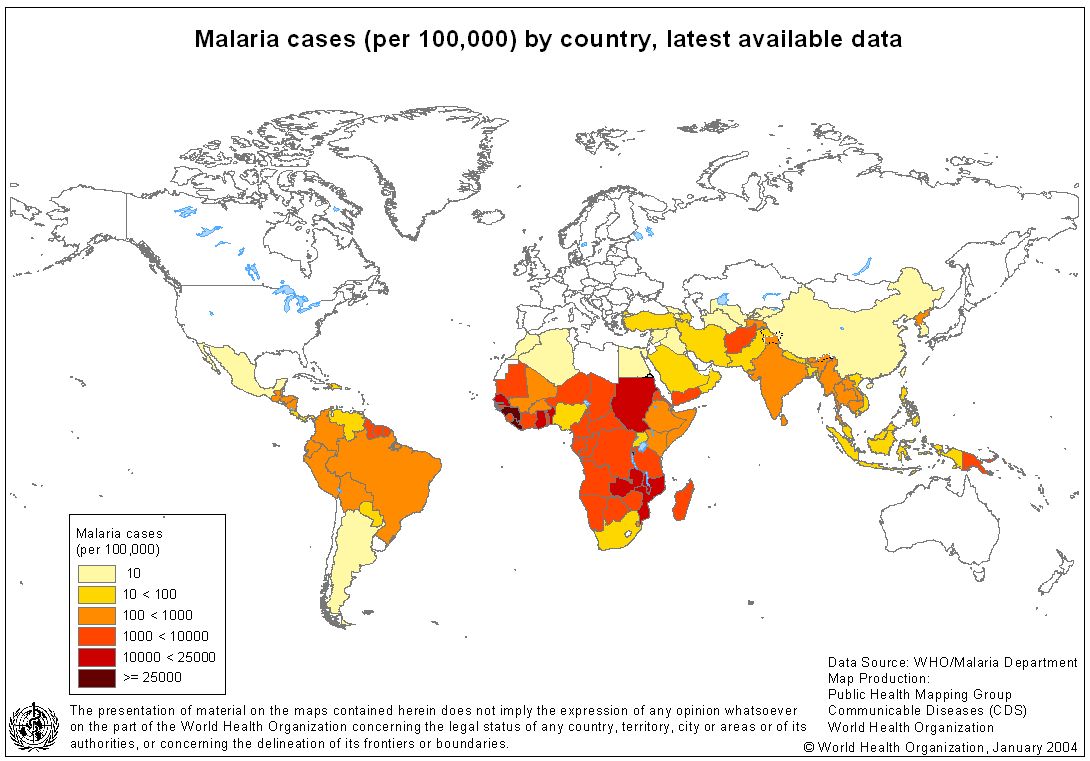
Malaria Control
Malaria control strategies:
- Early diagnosis and prompt treatment to cure patients and reduce parasite reservoir
- Vector control:
- Indoor residual spraying
- Long lasting insecticide treated bed nets
- Intermittent preventive treatment of pregnant women
Challenges in malaria control:
- Widespread resistance to conventional anti-malaria drugs
- Malaria and HIV co-infection
- Health Systems Constraints
- Access to services
- Coverage of prevention interventions
Malaria Geographic Distribution
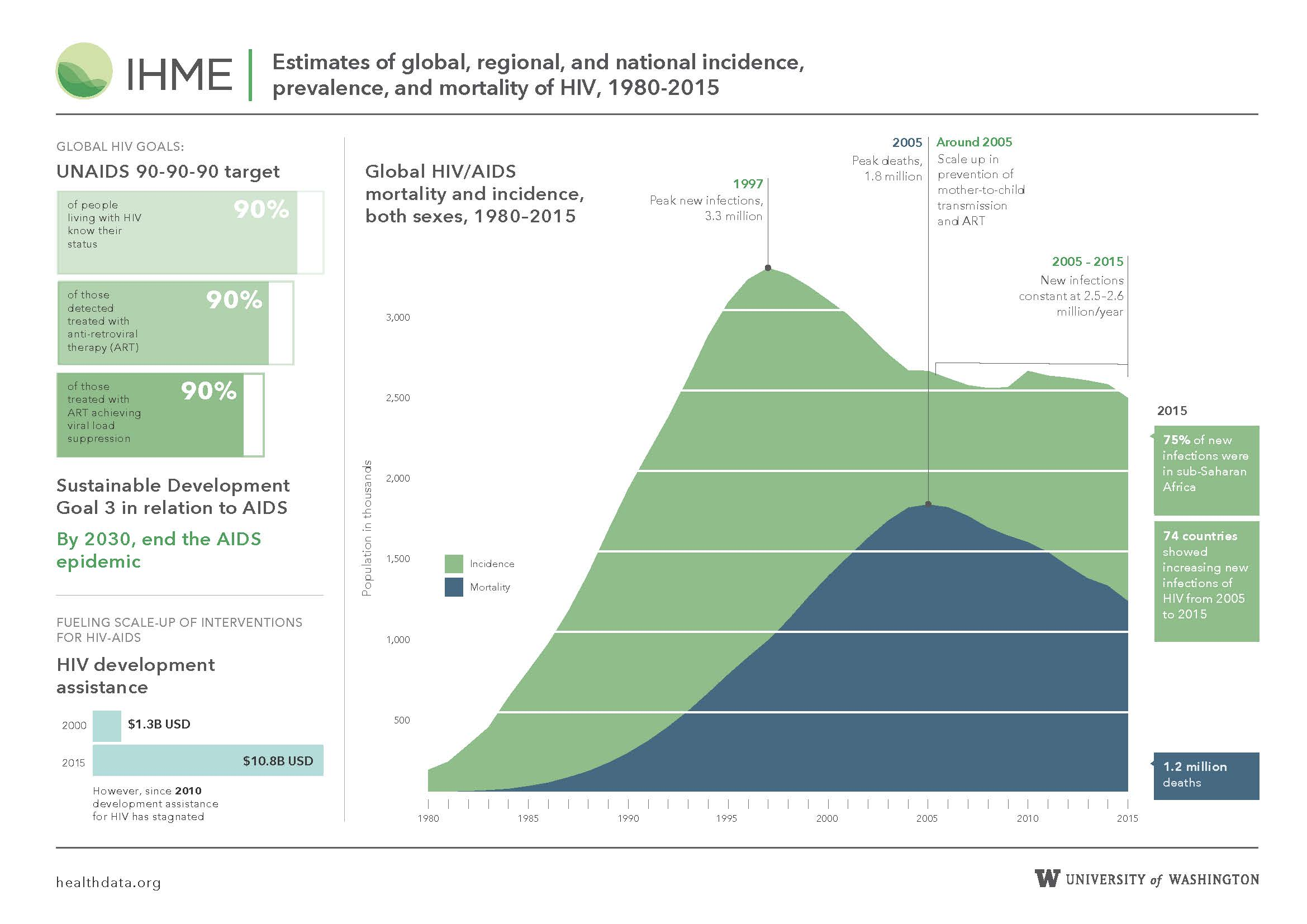
Global HIV Burden
39.9 million people living with HIV (2023)

HIV/AIDS
In 2023, 39.9 million people worldwide were living with HIV, of which 67% live in Sub-Saharan Africa
- 4.1 million people worldwide became newly infected
- 2.8 million people lost their lives to AIDS
New infections occur predominantly among the 15-24 age group.
First identified in the early 1980s. Has affected over 85 million people since the start of the epidemic.
Source: UNAIDS Global AIDS Update 2023
HIV Co-infections
Impact of TB on HIV:
- TB considerably shortens the survival of people with HIV/AIDS.
- TB kills up to half of all AIDS patients worldwide.
- TB bacteria accelerate the progress of AIDS infection in the patient
HIV and Malaria:
- Diseases of poverty
- HIV infected adults are at risk of developing severe malaria
- Acute malaria episodes temporarily increase HIV viral load
- Adults with low CD4 count more susceptible to treatment failure
Environmental Health
Air quality, water, and sanitation -- the areas where engineering interventions save the most lives.
Air Quality and Public Health
Sustainability Engineering Connection: Indoor and outdoor air pollution are among the largest environmental risk factors for human health. Engineers play a critical role in designing cleaner cookstoves, improving ventilation, and developing air quality monitoring systems.
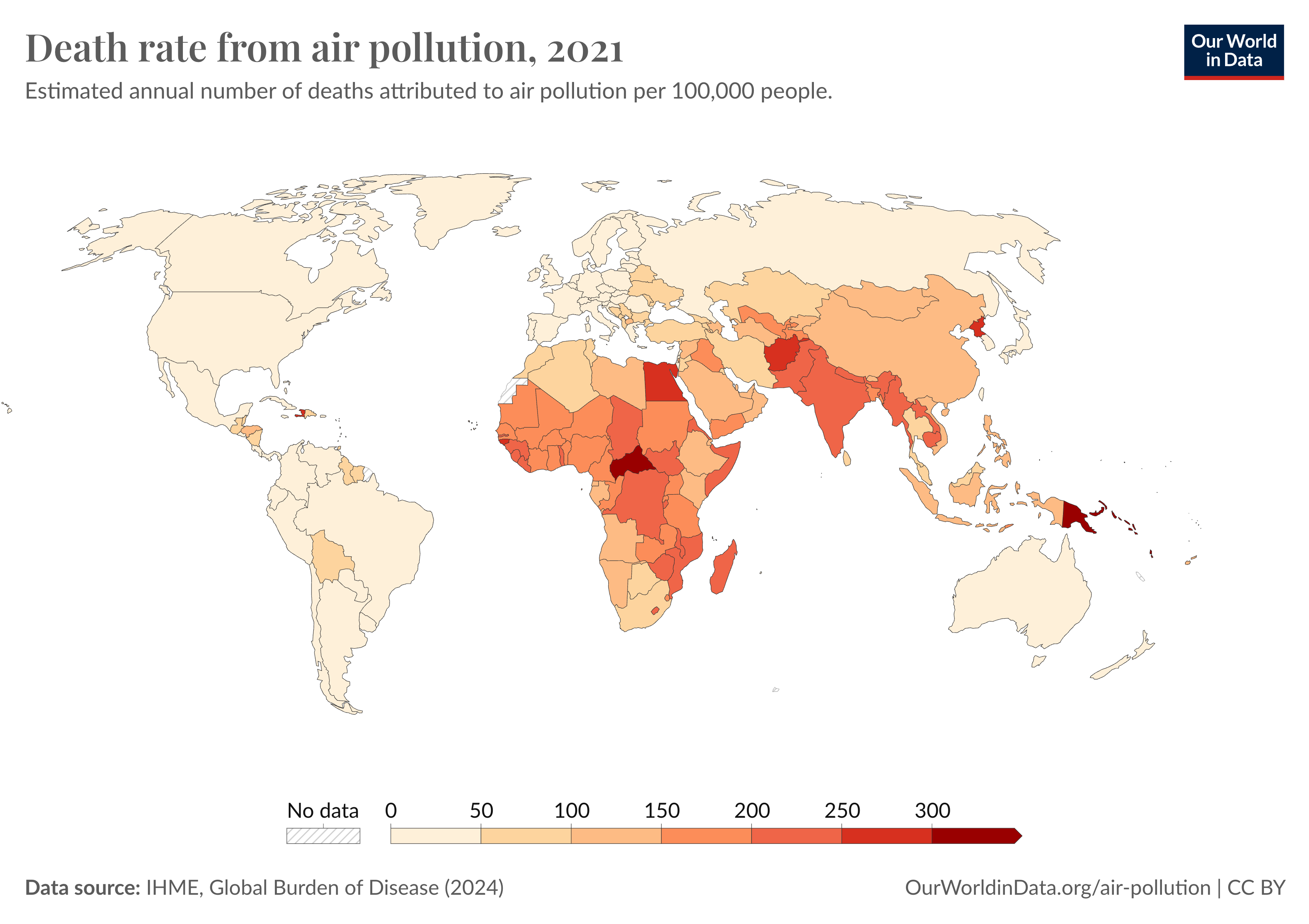
Water and Public Health
"No other single intervention in the history of medicine has saved as many lives and reduced as much suffering as the provisioning of uncontaminated water." — Paul Edward
One billion people in the world lack access to clean drinking water
- A leading cause of death worldwide
- An estimated 1.4 million people die each year from inadequate water, sanitation and hygiene
Source: WHO, 2023

Sanitation and Public Health
Minimum Standards:
- Safe disposal of excreta and sullage (greywater)
- Avoid disposal within 15 meters of any water source
- Provision of drainage
- Disposal of waste
- Control of insects and rodents


Thank You
EVEN 2909: Introduction to Sustainability Engineering — University of Colorado Boulder
Adapted from Global Health for Engineers, Mortenson Center in Global Engineering